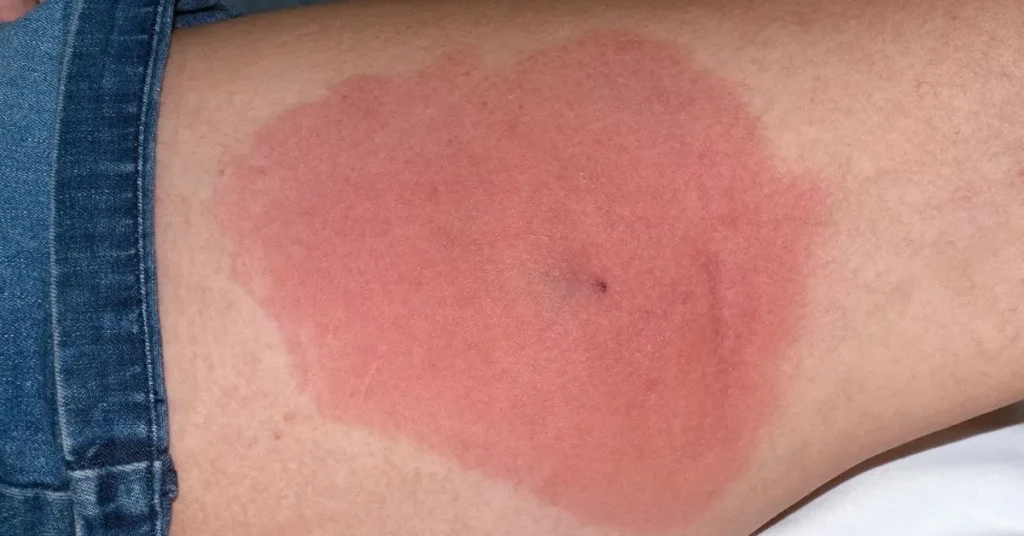
If you’ve noticed a red, painful bump on your skin and are wondering whether it could be MRSA, you’re not alone.
Many people search “what does MRSA look like” because early symptoms can resemble common skin problems like pimples, spider bites, or small boils.
MRSA stands for Methicillin-resistant Staphylococcus aureus, a type of staph bacteria that is resistant to several common antibiotics.
According to the Centers for Disease Control and Prevention, MRSA infections often begin as small red bumps that can quickly become swollen, warm, painful, and filled with pus.
Understanding what MRSA looks like in its early and later stages can help you recognize warning signs sooner.
In this guide, you’ll learn how to identify common symptoms, how MRSA differs from other skin infections, and when it’s important to seek medical care.
What Is MRSA?
MRSA, short for Methicillin-resistant Staphylococcus aureus, is a strain of staph bacteria that has developed resistance to many commonly used antibiotics. This resistance makes MRSA infections more difficult to treat than standard staph infections. Staph bacteria are normally present on the skin or in the nose of healthy individuals without causing harm. However, when the bacteria enter the body through cuts, scrapes, or other breaks in the skin, they can cause infections ranging from mild skin irritations to serious, potentially life-threatening conditions.
There are two main types of MRSA infections: community-acquired MRSA (CA-MRSA) and hospital-acquired MRSA (HA-MRSA). Community-acquired MRSA typically affects otherwise healthy people and often appears as red, swollen, and painful skin bumps, sometimes filled with pus or other drainage. These infections are usually localized but can spread if not treated promptly. Hospital-acquired MRSA, on the other hand, occurs in patients with weakened immune systems, often in surgical wounds or invasive devices like catheters, and can lead to more severe complications such as bloodstream infections or pneumonia.
Early recognition is crucial. According to the Mayo Clinic, MRSA skin infections often start as a small red bump resembling a pimple or insect bite. The affected area may feel warm, tender, and increasingly painful. Unlike ordinary pimples or minor skin irritations, MRSA bumps can grow quickly, become filled with pus, and may require medical attention for proper drainage and antibiotic treatment. Understanding MRSA’s characteristics and recognizing early signs can help prevent complications and reduce the risk of spreading the infection to others.
What Does MRSA Look Like on the Skin?
MRSA infections typically begin as small, red bumps on the skin that can easily be mistaken for pimples, insect bites, or minor skin irritations. These bumps are often painful, tender to the touch, and may feel warm as the infection develops. One of the hallmark signs of MRSA is that the bump can grow quickly and may fill with pus or other fluid, forming a boil or abscess. The surrounding skin often becomes red and inflamed, and in some cases, the area may ooze or crust over.
In many cases, MRSA lesions are solitary, but multiple bumps can appear in the same area or spread to other parts of the body. Common locations for MRSA skin infections include the legs, arms, armpits, groin, and buttocks, though they can appear anywhere on the body. People may also notice swelling around the infected area and a gradual increase in pain or discomfort over time.
It’s important to differentiate MRSA from other skin conditions. Unlike a typical pimple, MRSA bumps tend to grow more rapidly and may produce a yellow or white center due to pus accumulation. They can also be accompanied by a low-grade fever or general malaise in more severe cases. According to the Centers for Disease Control and Prevention, early identification and medical evaluation are crucial because untreated MRSA infections can worsen and, in rare cases, lead to systemic infections.
Recognizing the visual signs of MRSA on the skin redness, swelling, pain, and pus-filled bumps can help individuals seek treatment promptly, reducing the risk of complications and preventing the infection from spreading to others.
Early Signs of MRSA Infection
Recognizing the early signs of MRSA (Methicillin-resistant Staphylococcus aureus) is crucial for timely treatment and preventing complications. In its initial stages, MRSA often appears as a small red bump on the skin, resembling a pimple, insect bite, or minor scratch. While it may look harmless at first, these bumps tend to grow quickly, become increasingly tender, and can develop into painful, swollen areas. The skin around the infection may feel warm to the touch, indicating inflammation and the body’s immune response.
Another common early sign is the formation of pus or other drainage within the bump. Unlike ordinary pimples that may dry out naturally, MRSA lesions often continue to enlarge and fill with fluid. The center may appear yellow or white, and crusting can occur as the infection progresses. Some individuals may notice that the bump is firm or raised compared to the surrounding skin, and it may remain sensitive or sore even when not touched.
MRSA can affect people of all ages, but those with weakened immune systems, recent skin injuries, or close contact with infected individuals are at higher risk. Early warning signs may also include mild fever, fatigue, or general discomfort if the infection is spreading. According to the Mayo Clinic, catching these early symptoms and seeking medical care promptly can prevent the infection from becoming severe, reduce the risk of spreading to others, and improve treatment outcomes.
Being vigilant for red, swollen, painful bumps that grow rapidly, especially with pus or crusting, is the first step in identifying a possible MRSA infection and taking immediate action to address it.
MRSA vs Spider Bite: How to Tell the Difference
MRSA infections and spider bites can look remarkably similar at first, which often causes confusion. Both may appear as red, swollen bumps on the skin, sometimes with pain or tenderness. However, there are key differences that can help identify whether a skin lesion is more likely MRSA or a spider bite.
MRSA bumps typically develop rapidly and are often filled with pus or other fluid. The center of the lesion may appear yellow or white, and the surrounding skin can be warm, red, and inflamed. Pain tends to increase quickly, and multiple bumps may appear nearby if the infection spreads. In contrast, most spider bites, except those from venomous species like the brown recluse, generally remain small, localized, and do not fill with pus. A spider bite may blister or form a small ulcer, but it usually does not progress into a large abscess without secondary infection.
Another distinguishing factor is systemic symptoms. MRSA infections, especially more severe ones, can be accompanied by fever, chills, or general malaise. Spider bites usually cause localized pain, mild swelling, and itching, with systemic symptoms being rare unless the bite is venomous. The history of exposure is also helpful MRSA can develop anywhere on the body, particularly areas prone to cuts, scrapes, or friction, whereas spider bites are often in exposed areas like arms, legs, or hands.
According to the Centers for Disease Control and Prevention, early evaluation by a healthcare professional is essential if there is uncertainty. Prompt identification ensures proper treatment, prevents the infection from worsening, and reduces the risk of MRSA spreading to others.
Stages of MRSA Infection
MRSA infections often progress through several stages, and recognizing these can help in identifying the infection early and seeking timely treatment. Understanding the stages also helps differentiate MRSA from minor skin irritations or other infections.
Stage 1: Small Red Bump
The infection typically begins as a small red bump, resembling a pimple, insect bite, or minor scratch. At this stage, the area may be slightly tender or itchy, and the bump may appear firm or raised compared to the surrounding skin. Early recognition is key, as this is when intervention can prevent further progression.
Stage 2: Swelling and Pus Formation
As MRSA develops, the bump becomes larger, more painful, and may fill with pus or other fluid. The surrounding skin often becomes red, warm, and inflamed. The bump may start to ooze or crust over, signaling that the body is actively responding to the bacterial infection.
Stage 3: Abscess and Drainage
In more advanced cases, the bump can form a full abscess a collection of pus trapped under the skin. The area may become increasingly tender, swollen, and warm. Drainage may occur naturally or require medical intervention to remove the pus safely. At this stage, patients may also experience fever, fatigue, or general discomfort, indicating that the infection could be spreading.
Stage 4: Healing
With proper treatment, including antibiotics and drainage if necessary, MRSA lesions eventually heal. The redness, swelling, and pain gradually subside, and the skin may leave a small scar or discoloration. Proper hygiene and wound care during healing are essential to prevent reinfection or transmission to others.
According to the Mayo Clinic, recognizing these stages early and seeking medical care promptly can reduce complications and ensure effective treatment.
When to See a Doctor
Knowing when to seek medical attention for a suspected MRSA infection is critical. While some minor skin irritations may resolve on their own, MRSA infections can progress rapidly and may lead to serious complications if left untreated. Immediate medical evaluation is recommended when a bump or lesion shows certain warning signs.
First, if the affected area is growing rapidly, increasingly painful, or filled with pus, it could indicate an advancing MRSA infection. Swelling, redness spreading beyond the initial bump, or warmth around the area are also red flags. Multiple lesions appearing close together or spreading to other parts of the body warrant prompt attention.
Other signs that require urgent care include fever, chills, fatigue, or general malaise, which may indicate that the infection is no longer confined to the skin and could be affecting the bloodstream. Additionally, the presence of red streaks radiating from the infected area or swelling of nearby lymph nodes can suggest a more serious systemic infection.
Individuals with weakened immune systems, chronic illnesses, or pre-existing skin conditions should be especially vigilant, as they are at higher risk for complications. Children, older adults, and people with surgical wounds or invasive devices such as catheters should also seek early evaluation.
According to the Centers for Disease Control and Prevention, early medical intervention improves treatment outcomes, prevents the infection from worsening, and reduces the risk of spreading MRSA to others. Even if symptoms seem mild, consulting a healthcare professional can help confirm the diagnosis and determine the most effective course of treatment.
How MRSA Is Diagnosed
Accurate diagnosis of MRSA (Methicillin-resistant Staphylococcus aureus) is essential to ensure proper treatment and prevent complications. Because MRSA can resemble other skin infections, healthcare professionals rely on specific tests and clinical evaluation to confirm its presence.
When you visit a doctor with a suspicious bump, boil, or abscess, the first step is usually a physical examination. The doctor will assess the size, color, warmth, and tenderness of the lesion and check for signs of spreading redness, pus, or inflammation. They may also ask about your recent health history, any previous infections, injuries, or exposure to someone with MRSA.
To confirm that the infection is caused by MRSA, a swab of the affected area is often taken. This sample is sent to a laboratory where it is cultured to identify the bacteria and test its resistance to antibiotics. Lab results typically indicate whether the infection is caused by regular Staphylococcus aureus or MRSA, which helps determine the most effective antibiotic for treatment.
In cases where the infection appears more severe or systemic, doctors may also order blood tests or other imaging tests to check if the bacteria have spread beyond the skin. Early and accurate diagnosis allows for targeted treatment, reducing the risk of worsening infection, hospitalization, or transmission to others.
According to the Mayo Clinic, timely diagnosis combined with appropriate medical care, including antibiotics and proper wound management, is the key to effectively treating MRSA and preventing complications. Recognizing the signs early and seeking professional evaluation ensures better outcomes and faster recovery.
Treatment Options for MRSA
Treating MRSA (Methicillin-resistant Staphylococcus aureus) requires a combination of medical care, antibiotics, and proper wound management. Because MRSA is resistant to many common antibiotics, it’s important to follow a doctor’s guidance to ensure effective treatment and prevent the infection from worsening or spreading.
For minor skin infections, doctors may recommend draining the abscess or boil. This procedure removes pus from the infected area and can speed healing. Sometimes, draining the infection is enough, but many cases also require antibiotic therapy. Healthcare providers prescribe antibiotics that are effective against MRSA, such as doxycycline, clindamycin, or trimethoprim-sulfamethoxazole. It’s essential to complete the full course of antibiotics, even if the infection appears to improve, to ensure all bacteria are eliminated.
In more severe or systemic cases, MRSA can spread to the bloodstream, lungs, or other organs. These infections may require hospitalization and intravenous antibiotics. Early intervention reduces the risk of complications such as sepsis, pneumonia, or organ damage.
Home care is also an important part of treatment. Keeping the infected area clean and covered, practicing good hand hygiene, and avoiding sharing personal items like towels or clothing can prevent MRSA from spreading to others. According to the Centers for Disease Control and Prevention, monitoring the infection for changes in size, redness, or pain is crucial. Patients should report any worsening symptoms promptly to their healthcare provider.
With proper medical care and hygiene practices, most MRSA skin infections heal without long-term complications. Early recognition and treatment are key to minimizing discomfort, preventing recurrence, and stopping the infection from spreading.
How to Prevent MRSA
Preventing MRSA (Methicillin-resistant Staphylococcus aureus) infections involves practicing good hygiene, maintaining a clean environment, and taking precautions to avoid exposure. Because MRSA spreads through direct skin-to-skin contact or contact with contaminated surfaces, simple daily habits can significantly reduce the risk of infection.
Hand hygiene is one of the most effective preventive measures. Washing hands thoroughly with soap and water, or using an alcohol-based hand sanitizer, helps eliminate bacteria that may be present after touching surfaces, wounds, or other people. Avoid touching cuts, scrapes, or open wounds with unwashed hands, and always clean minor skin injuries promptly with antiseptic solutions.
Covering wounds is another important step. Keep cuts, scrapes, and surgical incisions clean and covered with a sterile bandage until fully healed. This prevents bacteria from entering the skin and reduces the chance of spreading MRSA to others. Change bandages regularly and dispose of them safely.
Avoid sharing personal items like towels, razors, clothing, or sports equipment, as these can transfer bacteria from one person to another. In communal settings such as gyms, locker rooms, or dormitories, use barriers like clothing or towels when sitting on shared surfaces, and clean equipment before and after use.
Maintaining a clean living environment also helps prevent MRSA. Regularly disinfect frequently touched surfaces, including doorknobs, countertops, and gym equipment. Launder clothes, towels, and bedding in hot water to kill bacteria.
According to the Centers for Disease Control and Prevention, following these practices consistently can greatly reduce the risk of MRSA infection and its spread. Being vigilant about hygiene, wound care, and environmental cleanliness is essential for protecting yourself and others.
Frequently Asked Questions
Understanding MRSA (Methicillin-resistant Staphylococcus aureus) can help you identify symptoms early and take appropriate action. Here are some commonly asked questions about MRSA infections.
1. Is MRSA always painful?
Not always at first. Early MRSA may appear as a small red bump resembling a pimple or insect bite. Initially, it might be tender or itchy rather than severely painful. As the infection progresses, the area usually becomes increasingly painful and swollen.
2. Can MRSA go away on its own?
Minor skin infections sometimes resolve with proper hygiene and care, but MRSA is antibiotic-resistant, so many cases require medical treatment. Without proper care, MRSA can worsen, spread, or lead to serious complications.
3. How fast does MRSA spread?
MRSA can develop quickly. A small bump may enlarge within days, forming a painful abscess. Close skin-to-skin contact or shared personal items can increase the risk of transmission to others.
4. Can MRSA look like a bug bite or pimple?
Yes. Early MRSA often resembles a pimple, spider bite, or small scratch. Key differences include rapid growth, pus formation, and increasing pain. Multiple bumps or spreading redness are additional warning signs.
5. When should I see a doctor?
Seek medical care if the bump grows rapidly, becomes painful, shows pus or crusting, or is accompanied by fever or spreading redness. Early evaluation helps prevent complications and reduces the risk of spreading the infection.
6. How can I prevent MRSA?
Practice good hand hygiene, keep wounds clean and covered, avoid sharing personal items, and disinfect frequently touched surfaces. Early recognition and preventive measures are essential for protecting yourself and others.
According to the Centers for Disease Control and Prevention, following these precautions and seeking timely medical care are key to effectively managing and preventing MRSA infections.
Conclusion
Recognizing what MRSA looks like is critical for protecting your health and preventing the infection from spreading to others.
MRSA (Methicillin-resistant Staphylococcus aureus) often starts as a small red bump that can resemble a pimple, insect bite, or minor scratch. Early signs include redness, swelling, tenderness, and sometimes pus or fluid in the lesion.
If left untreated, MRSA can progress rapidly, forming painful abscesses, spreading to other areas of the body, and in severe cases, causing systemic infections that require urgent medical care.
Understanding the differences between MRSA and other skin issues, such as spider bites or ordinary pimples, helps you identify infections early.
Paying attention to warning signs rapid growth, increasing pain, pus formation, spreading redness, or fever can prompt timely medical intervention.
According to the Mayo Clinic, early diagnosis, appropriate antibiotic treatment, and proper wound care are key to managing MRSA effectively and preventing complications.
Prevention is equally important. Practicing good hand hygiene, keeping wounds clean and covered, avoiding shared personal items, and maintaining a clean environment are simple yet effective steps to reduce your risk.
By staying vigilant and acting promptly when signs appear, you can minimize the impact of MRSA infections and protect both yourself and those around you.
Early awareness, proper treatment, and preventive habits together provide the best strategy against MRSA.

Jordon Fox is an emerging artist and creative from Philadelphia, Pennsylvania, known for blending music, fashion, and fitness into his personal brand and artistic identity. He’s built a reputation as a multi-talented creator with a strong focus on authenticity and inspiring others.